► Start of the game
Atishoo! The die is cast. At speeds of up to 160 kilometers per hour, a patient in the waiting room emits a cloud of tiny spittle droplets, which serve as a means of transport for pathogens from the throat or respiratory tract. And with that, our first player moves up a square. The influenza virus, or the real flu. The 80 to 120 nanometer small viruses are protected by the liquid envelope, ejected from the throat – directly onto the patient’s hand.
All squares are now occupied. Alongside the new arrivals, the pawns of Rota, Noro and Adenoviruses are already in the game. These viruses cause diarrheal diseases. Poor hand hygiene can allow them to adhere to the infected person’s hand. It is precisely this lack of hygiene that allows them to advance up the board. Because the patient – ignoring the need to disinfect the contaminated hand – stands up to shake his doctor’s hand. In this encounter, the pathogens can migrate from the patient’s hand to that of the doctor. This move is referred to as a contact or smear infection. Thanks to this person-to-person transmission, influenza has almost reached its destination. If the doctor now takes part in an operation, the pathogens have won.
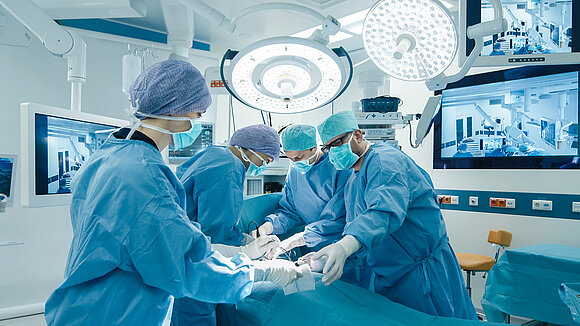
However, well-trained hospital staff know the dangers of direct contact. The Robert Koch Institute (RKI) estimates that around 90 percent of pathogens are transmitted via the hands. After contact with rooms or patients that are likely to be contaminated, hospital staff therefore pay particular attention to their hand hygiene. Surgical hand disinfection avoids spreading pathogens over the body and thoroughly cleans the forearms. In this way, the staff not only protect patients, but also themselves. For the pawns in the influenza game, it’s all over at this point. But at the start, more influenza viruses have sneaked onto the playing field unnoticed.